19.3 Retinal and Choroidal Biopsy for Choroidal Tumours
- Diagnostic uncertainty
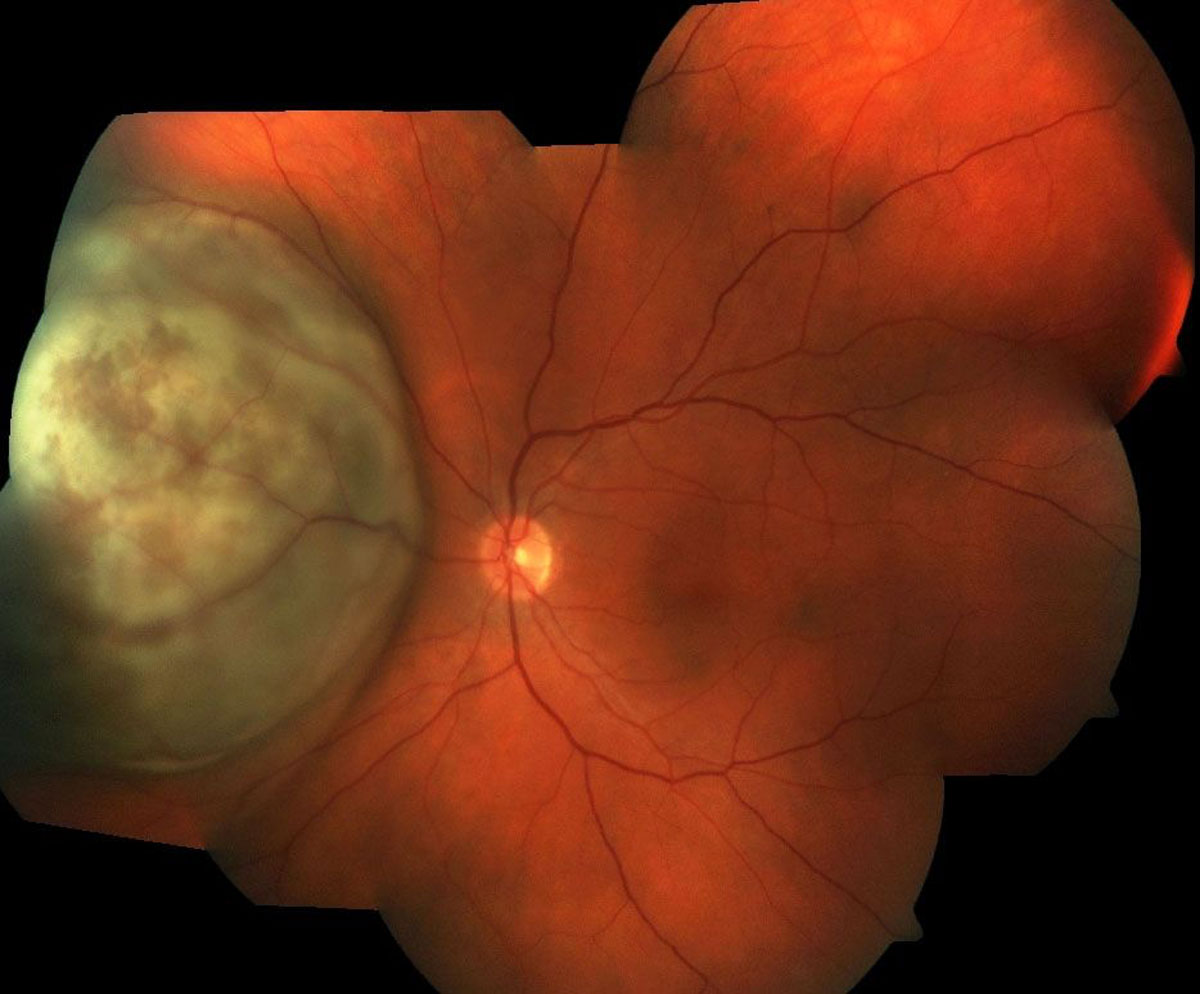
- Melanoma prognostication (Figure 19.3.1)
- Retinoblastoma, because of risk of tumor seeding
- Hemangioma, because of risk of bleeding
- Significant retinal detachment overlying the tumor
Johnston RL, Tufail A, Lightman S, Luthert PJ, Pavesio CE, Cooling RJ, Charteris D. Retinal and choroidal biopsies are helpful in unclear uveitis of suspected infectious or malignant origin. Ophthalmology 2004; 111:522-528.
Preparation
Liaise with laboratory to ensure that:
- The cytologist or pathologist is prepared to deal with the specimen and invited to the operating room to check the sample
- Correct transport medium is used (e.g., Cytolyt® solution; RPMI)
There are two main approaches to choroidal biopsy:
A. Trans-Vitreoretinal (Via Pars Plana)
- Using the vitreous cutter
- Fine Needle Aspiration Biopsy (FNAB)
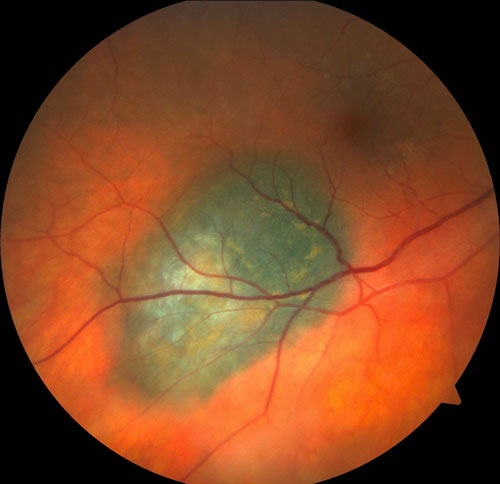
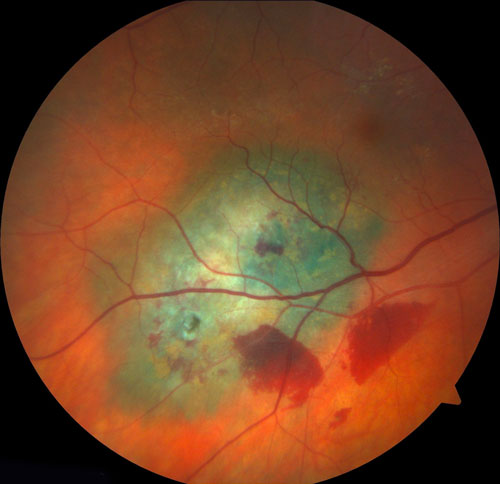
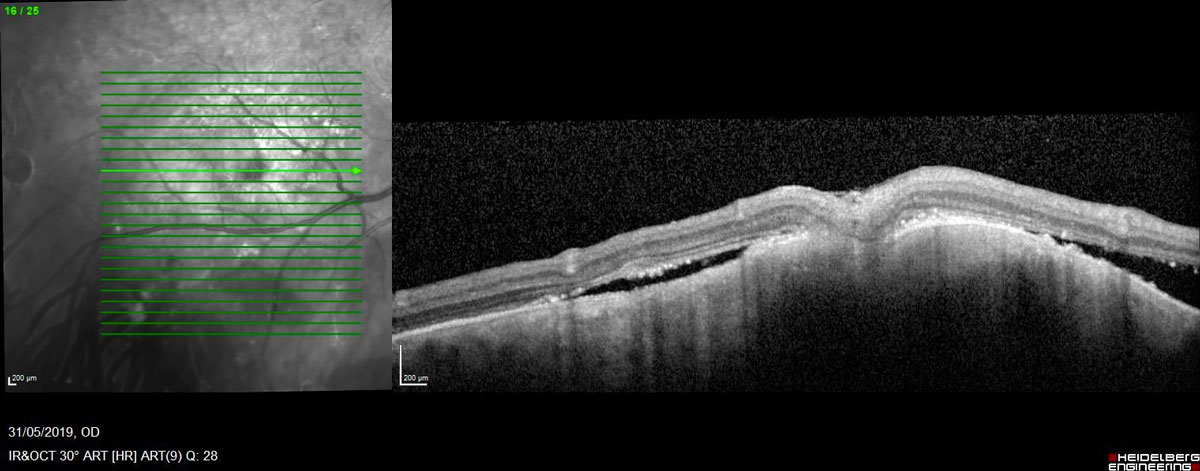
The trans-vitreoretinal approach is best for posterior tumors (Figure 19.3.2, Figure 19.3.3 and Figure 19.3.4).
Using a vitreous cutter has the following advantages: Direct (rather than inverted) visualization, control of intra-ocular pressure for hemostasis, usually able to obtain a larger specimen.
FNAB has the following advantages: Cost-saving, avoids cataract (although this is not an issue if the vitreous cutter is used with minimal vitrectomy), the bore of the needle is perpendicular to the retinal plane, unlike the cutter port which is parallel.
Figure 19.3.3 Same Lesion Figure 19.3.2 Immediately After a Trans-pars plana Choroidal Biopsy with a 27-gauge Vitrectomy System
B. Trans-Scleral
- Fine Needle Aspiration Biopsy (FNAB)
- Incisional
The trans approach is best for anterior tumors.
FNAB has the following advantages: Simpler, less complications such as hemorrhage.
Incisional has the following advantages: Able to obtain a larger specimen.
i. Vitreous-Cutter Biopsy
- Use a 27-gauge (or smaller) vitrectomy system
- Prime the vitrectomy system without fluid in the cutter line. If using the Alcon CONSTELLATION® vision system: The "Setup" screen is divided into 6 boxes. The top middle box says "Probe." In this box it says "Skip Prime". Push the button next to this and it will place a green check next to it. When everything on the machine is set up and ready to prime, just select "Start Prime" as normal. The whole system will prime like normal except there will be no fluid in the cutter line, allowing for a pure sample to be taken
- Setup the specimen collection. Separate the connectors on the blue aspiration tubing behind the vitrectomy cutter. A syringe can be directly attached to the aspiration line (and aspirated by an assistant during vitrectomy), but a more elegant technique is to attach a collection tube in a “closed-loop” system. Find the white adaptor from the pack contents and connect it to the blue connector closest to the vitrectomy cutter. Place a collection tube (e.g. for blood typing) in a sterile plastic bag and tie the end of the bag off to keep the setup sterile (alternatively, a sterile collection tube can be used). Insert two 19-gauge needles through the bag into the collection tube. Attach the ends of the separated aspiration line to the 19-gauge needles (Figure 19.3.5)
- Set-up as for a standard 3-port, 27-gauge vitrectomy procedure
- Consider elevating the intra-ocular pressure (IOP) if the tumor is prone to bleed
- Pass the vitrectomy cutter through the retina into the tumor, avoiding retinal vessels and rotating the cutter so that the port faces the tumor
- Start with maximum suction (650 mmHg) and a low cutting rate (100 - 200 cpm)
- Rotate the cutter to obtain the maximal volume of specimen (Figure 19.3.6)
- If hemorrhage occurs, raise the IOP until it stops. This is particularly prone to occur at the time the vitrector cutter is withdrawn from the tumor
- Remove the cutter from the tumor, increase the cutting rate to maximum and cut / aspirate a minimal amount of vitreous to flush the sample up the tube. This is also important to lower the IOP if it has been raised (since the infusion line will not have been cleared of vitreous, the IOP will not fall even if the infusion pressure is lowered). It is important to ensure that the central retinal artery is perfused prior to completing the case
- Withdraw the vitrectomy instruments from the eye
- Check the collection tube (or syringe) to ensure sufficient specimen has been collected
- If insufficient specimen has been collected, a second pass of the tumor can be performed, with the same or a new collection tube
- Once sufficient specimen has been obtained, the collection tube, bag and two 19-gauge needles can be removed from the setup and passed to an assistant or scout nurse. If necessary, transport medium (e.g. RPMI) can be added directly to the collection tube
- The specimen should be sent directly to the cytopathologist, on ice if necessary (discuss timing, transportation and media prior to the case)
- Remove the cannulae. It is not required to perform further vitrectomy or induce a PVD
- Apply triple freeze-thaw cryotherapy to the sclerotomies to minimize the risk of tumor seeding. Sclerotomy suturing is not usually necessary
All rights reserved. No part of this publication which includes all images and diagrams may be reproduced, distributed, or transmitted in any form or by any means, including photocopying, recording, or other electronic or mechanical methods, without the prior written permission of the authors, except in the case of brief quotations embodied in critical reviews and certain other noncommercial uses permitted by copyright law.
Westmead Eye Manual
This invaluable open-source textbook for eye care professionals summarises the steps ophthalmologists need to perform when examining a patient.